
Dropping the Mic on Telecoils
Justin R. Burwinkel, Au.D., Maddie Olson, Au.D., and Lori Rakita, Au.D.
Discussion of key research findings regarding the recommendation and demonstration of hearing loops
Background
It is well documented that as hearing loss worsens, the signal-to-noise ratio (SNR) required to accurately recognize speech also increases (Killion et al., 2004). This difficulty may contribute to listening fatigue and the avoidance of difficult listening situations like group meetings, lectures, religious services, and theater. Even with carefully fit amplification and directional microphones, patients may still have difficulty understanding speech in these types of complex listening environments. There are numerous wireless assistive listening technologies available which help to effectively improve the SNR for the patient. Hearing aids and cochlear implants can be wirelessly connected to remote microphones using various types of wireless technologies, including infrared systems, FM systems, 2.4GHz wireless protocols, and induction hearing loops via a telecoil setting. It is important for clinicians to not only understand the realistic and relative efficacy of these systems (Rodemerk & Galster, 2015), but also factors that impact their patients’ awareness and utilization of these systems.
Hearing loops, which have been used as public assistive listening systems for decades, have been trumpeted by many as “the preferred assistive listening technology” for their convenience, reliability, cosmetic discretion, and ease of use (Kaufmann et al., 2015). The quality of hearing loop installations has greatly improved since adoption of the IEC-60118-4 standard, which added controls for ensuring low magnetic background noise, a calibrated field strength level, and uniform coverage within each venue.
Most public venues are now required by law to make hearing assistive technology (HAT) available. These laws also require options for hearing aid and cochlear implant compatibility by using either hearing loop installations or neck loop adapters for systems that otherwise offer handheld receivers. When compared to listening devices with headphones or earbuds, hearing aid compatibility provides HAT users with direct-audio-input amplification that has been fine-tuned for each user’s own unique ranges of hearing ability through the use of their own hearing aids in conjunction with the assistive listening system (Kaufmann et al., 2015).
Recently-published best practices guidelines for the management of patients with severe and profound hearing loss also implore that, “Unless contraindicated, the hearing care professional should activate the [telecoil function for the patient]…and arrange for the client to experience a good working inductive loop, as this remains the most widespread and effective way to hear well in public spaces” (Turton et al., 2020). However, clinicians may still have questions about how to integrate the various assistive listening technologies into their patients’ treatment plans and counseling.
We conducted a series of studies to assess the degree of patient benefit when using a remote microphone or the telecoil function of their hearing aids, as well as the efficacy of different counseling approaches related to the use of telecoils with hearing loops. For our studies, we recruited a total of 28 participants representing a wide range of hearing impairment; 14 individuals evaluated the Starkey Evolv AI Power Plus BTE 13 with embedded telecoils and another 14 individuals evaluated the Evolv AI wireless CIC that could use the telecoil input function of Starkey’s Remote Microphone + 2.4GHz wireless accessory. The studies included lab-based speech recognition tests as well as a field trial. The field trial culminated in a simulated movie theater and auditorium listening experience where the researchers observed the behavior of participants in addition to collecting their feedback.
Here’s what we learned:
1. Patients can enjoy dramatic improvement from using hearing assistive technology
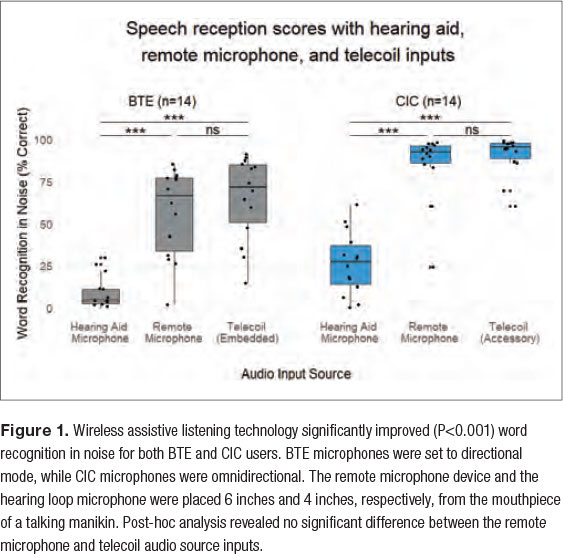 By moving the microphone closer to the target speaker, HAT can greatly improve the SNR for the patient. To measure the maximal degree of potential benefit of remote microphones and a telecoil setting with hearing loops, we designed a laboratory study where we expected performance to be poor using the hearing aid microphone alone. AzBio sentences were presented to the participants at 65 dBA, with a +10dB SNR. However, the participants were seated 3 meters from the talking mannikin, in a reverberant room that had a critical distance of only 1.5 meters.
By moving the microphone closer to the target speaker, HAT can greatly improve the SNR for the patient. To measure the maximal degree of potential benefit of remote microphones and a telecoil setting with hearing loops, we designed a laboratory study where we expected performance to be poor using the hearing aid microphone alone. AzBio sentences were presented to the participants at 65 dBA, with a +10dB SNR. However, the participants were seated 3 meters from the talking mannikin, in a reverberant room that had a critical distance of only 1.5 meters.
For both the BTE Group (n=14) and CIC Group (n=14), we found statistically significant improvements (P<0.001) in aided speech recognition in noise scores, while using the remote microphone and telecoil settings, when compared to the standard hearing aid microphone condition (Figure 1). There were no statistical differences between the remote microphone and the telecoil conditions, for either group.
2. Counseling on telecoil use does not need to be extensive to be effective
 In their step-by-step guide to looping a community, Lopez & Caccavo (2014) strongly urged hearing healthcare professionals to provide patients and their companions with demonstrations of a hearing loop during office visits. We were curious how different levels of professional intervention affect hearing aid users’ understanding, awareness, and use of telecoils with hearing loops, when available.
In their step-by-step guide to looping a community, Lopez & Caccavo (2014) strongly urged hearing healthcare professionals to provide patients and their companions with demonstrations of a hearing loop during office visits. We were curious how different levels of professional intervention affect hearing aid users’ understanding, awareness, and use of telecoils with hearing loops, when available.
To test these effects, we split our BTE Group (n=14) into two, randomly selected subgroups: Demo Group (n=7) and No Demo Group (n=7). Both the Demo Group and No Demo Group were provided a dedicated telecoil setting. At the time of their initial hearing aid fittings, the No Demo Group received informational counseling regarding the telecoil setting and were shown the hearing accessibility signage (Figure 2) found in public venues where they may want to use the telecoil setting. The Demo Group, in addition to informational counseling, was also provided a brief, interactive demonstration of the telecoil functionality. The demonstration allowed the participants to practice accessing the hearing loop with their telecoil setting and then listen to a short video clip that was otherwise silent to others in the room. Participants in the Demo Group were also given a list of local venues with permanently installed hearing loops and were encouraged to experience listening in one of the hearing loops on their own.
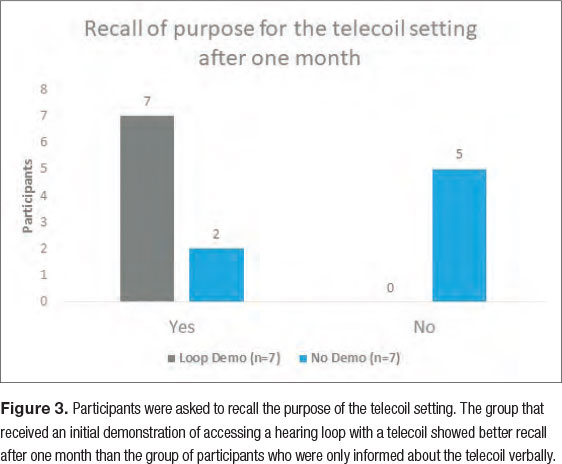 When the participants returned one month later, the researchers interviewed each participant to assess their knowledge retention regarding the purpose of the telecoil setting that they were provided with and how they would access it. Even after just one month, we observed notable differences in knowledge retention between the two groups (Figure 3); only 29 percent of the No Demo Group participants correctly recalled the purpose of their telecoil setting compared to the unanimous (100 percent) recall among the Demo Group participants.
When the participants returned one month later, the researchers interviewed each participant to assess their knowledge retention regarding the purpose of the telecoil setting that they were provided with and how they would access it. Even after just one month, we observed notable differences in knowledge retention between the two groups (Figure 3); only 29 percent of the No Demo Group participants correctly recalled the purpose of their telecoil setting compared to the unanimous (100 percent) recall among the Demo Group participants.
At the two-month mark, participants were asked to return for a simulated movie theater event hosted in Starkey’s professionally sound-designed Austin Theatre. This auditorium has a permanent hearing loop with the International Symbol of Access for Hearing Loss signage (Figure 2) clearly visible outside its entrance doors. For the simulated movie theater event, participants were instructed to use the hearing aid settings they felt would allow them to hear their best, but they were not specifically reminded to consider switching to the telecoil setting.
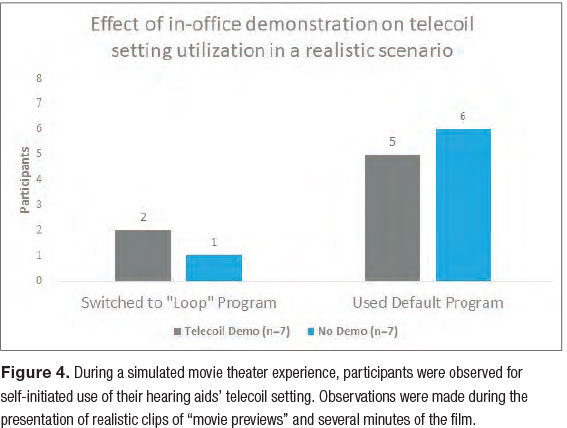 For the first five minutes of the film presentation, each participant was observed by a researcher to monitor and document the participants’ self-selected hearing aid settings. During this user-behavior observation period, we found that only three of the 14 BTE users (16.5 percent) utilized their telecoil setting unprompted (Figure 4). While we found more participants from the Demo Group self-selecting the telecoil setting than from the No Demo Group, this difference was negligible.
For the first five minutes of the film presentation, each participant was observed by a researcher to monitor and document the participants’ self-selected hearing aid settings. During this user-behavior observation period, we found that only three of the 14 BTE users (16.5 percent) utilized their telecoil setting unprompted (Figure 4). While we found more participants from the Demo Group self-selecting the telecoil setting than from the No Demo Group, this difference was negligible.
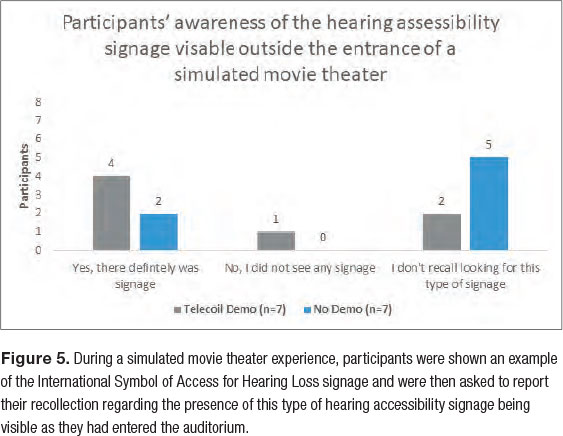 Interestingly, despite not showing significant differences in telecoil utilization, we did observe persisting disparities in information retention about the telecoil function and awareness of the hearing accessibility signage outside the entrance of the room. When the movie was stopped, following the five-minute user-behavior observation period, participants were, again, shown an image of hearing accessibility signage indicating telecoil compatibility with the sound system. The participants were then individually surveyed to assess their confidence in whether or not this type of signage was present when they had entered the simulated theater (Figure 5). The participants were also given the option to indicate that they did not remember looking for that type of signage.
Interestingly, despite not showing significant differences in telecoil utilization, we did observe persisting disparities in information retention about the telecoil function and awareness of the hearing accessibility signage outside the entrance of the room. When the movie was stopped, following the five-minute user-behavior observation period, participants were, again, shown an image of hearing accessibility signage indicating telecoil compatibility with the sound system. The participants were then individually surveyed to assess their confidence in whether or not this type of signage was present when they had entered the simulated theater (Figure 5). The participants were also given the option to indicate that they did not remember looking for that type of signage.
Participants from the No Demo Group more frequently reported not having looked for the hearing accessibility signage than the participants in the Demo Group, but a larger sample size would be needed to determine whether the difference between groups was statistically significant. Nevertheless, results of this survey provide useful insights regarding in-office demonstrations and counseling regarding use of wireless assistive listening technology. In our sample, the participants’ apparent awareness of hearing accessibility signage at the entrance of the simulated theatre did not translate into improved telecoil utilization in this realistic listening scenario.
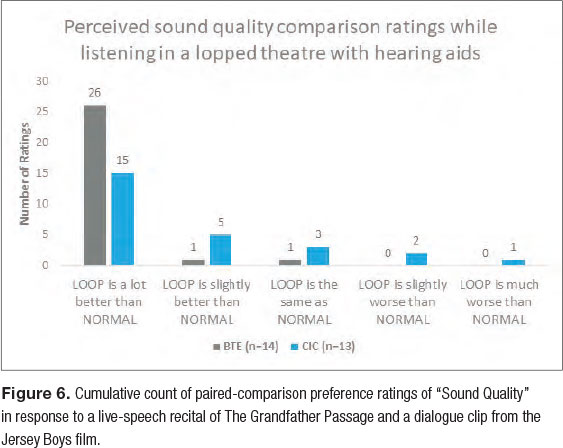 It is worth noting that, throughout the rest of the two-hour movie theater and auditorium listening event, we had participants conduct paired-comparison ratings of their microphone and telecoil user settings in response to numerous stimuli, including a live-speech narration of a passage and movie clip dialogue. Subjective ratings from both BTE and CIC hearing aid users (Figure 6) showed a clear preference for the telecoil setting. In addition, a preference assessment (Figure 7) indicated that most of the hearing aid users in our study desired to use hearing loops, on their own, after the study. Interpreting these results, we believe greater exposure to comparative listening experiences may be necessary for patients to appreciate their personal benefit from using the telecoil and to ultimately lead to lasting behavior change.
It is worth noting that, throughout the rest of the two-hour movie theater and auditorium listening event, we had participants conduct paired-comparison ratings of their microphone and telecoil user settings in response to numerous stimuli, including a live-speech narration of a passage and movie clip dialogue. Subjective ratings from both BTE and CIC hearing aid users (Figure 6) showed a clear preference for the telecoil setting. In addition, a preference assessment (Figure 7) indicated that most of the hearing aid users in our study desired to use hearing loops, on their own, after the study. Interpreting these results, we believe greater exposure to comparative listening experiences may be necessary for patients to appreciate their personal benefit from using the telecoil and to ultimately lead to lasting behavior change.
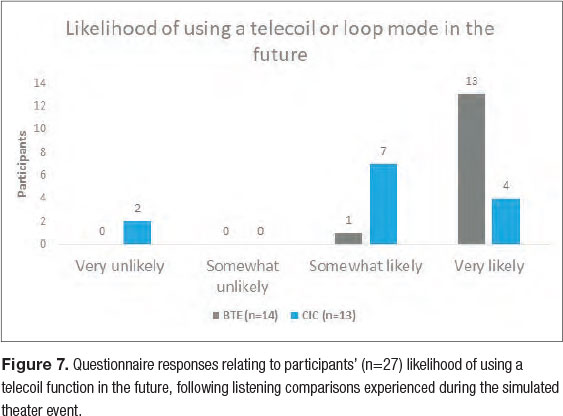 To those ends, we recommend providing patients with a hearing loop demonstration that yields an appreciably-different listening experience between the standard microphone setting and the telecoil setting. When selecting content for your demonstrations, consider that a post-hoc analysis of our data revealed the greatest differences in self-assessed speech intelligibility were when the participants watched clips from a British film. Similar to the waiting area of a typical clinic, these results were obtained in a situation where the room acoustics were favorable and other distractions were minimal. However, speech that is presented in an accent that is unfamiliar to the listener will inherently increase cognitive load and allow subtle SNR improvements to yield more appreciable differences in listening effort (Van Engen & Peelle, 2014).
To those ends, we recommend providing patients with a hearing loop demonstration that yields an appreciably-different listening experience between the standard microphone setting and the telecoil setting. When selecting content for your demonstrations, consider that a post-hoc analysis of our data revealed the greatest differences in self-assessed speech intelligibility were when the participants watched clips from a British film. Similar to the waiting area of a typical clinic, these results were obtained in a situation where the room acoustics were favorable and other distractions were minimal. However, speech that is presented in an accent that is unfamiliar to the listener will inherently increase cognitive load and allow subtle SNR improvements to yield more appreciable differences in listening effort (Van Engen & Peelle, 2014).
We also suggest challenging your patients to compare their telecoil setting to their standard microphone setting, in realistic situations that are relevant to them. Ding et al. (2015) previously reported that individuals with sensory handicaps found assistive technology demonstrations with clinicians to be beneficial for “learning the basics,” but were limited in allowing the patient to experiment thoroughly in a range of scenarios they deemed important. We conducted our study in the midst of the COVID-19 pandemic, so many of our participants did not attempt to use the telecoil setting on their own, as it would have required them to visit public places they otherwise would not have visited during that time.
We believe that this likely explains why the participants who had retained knowledge of the telecoil function and were aware of the hearing accessibility signage still failed to switch their hearing aids into the telecoil setting. Even though they were listening in a scenario where they apparently could have benefited from doing so, they were not motivated by awareness alone. After two hours of experience, comparing the telecoil setting to the standard microphone setting during the simulated movie theater event, participants began to appreciate the differences and, consequently, indicated a likelihood to request and use hearing aids with telecoils in the future.
3. Candidacy for HAT is wider than expected
The current consensus practice guidelines include the recommendation that clinicians activate telecoil functions for patients with severe and profound hearing loss as hearing loops remain “the most widespread and effective way to hear well in public spaces” (Turton et al., 2020). However, there has been some ongoing debate about the appropriateness of activating telecoils for patients with mild and moderate degrees of hearing loss, where the patients’ SNR impairments may be less severe and the overall benefit of the telecoil input could be diminished by using larger vent sizes.
We were interested in developing a better understanding of the candidacy criteria for not only telecoils, but all forms of assistive listening technology. We designed a variety of experiments to compare the relative performance of hearing aid users listening with a standard hearing aid microphone input, a telecoil input, and a remote microphone input. The wireless functionality of the Evolv AI CIC allows them to be wirelessly paired with the multi-function Remote Microphone + 2.4GHz accessory, which has a selectable audio input option that can provide access to hearing loops in addition to operating as a traditional remote microphone device. For all our testing, the ear coupling and amplification settings were the same as what the participants used during extended field evaluation of the devices, between study sessions.
We conducted a Pearson correlation analysis to determine whether any single audiologic test was associated with the degree of perceived speech intelligibility improvement, while using a telecoil function, during the two-hours of paired-comparison listening that was conducted in the sound treated auditorium. Neither pure-tone average (PTA) nor high-frequency pure-tone average (HF-PTA) were significantly associated with the participants’ degree of self-reported speech intelligibility improvement. There was also not a significant relationship with results of cognitive screening using the Montreal Cognitive Assessment (MoCA) tool. Nevertheless, we did observe a significant, strong association with the participants’ SNR Loss, as measured with the QuickSIN (r=0.589, 95% CI 0.269 to 0.792, P=.001), and a significant moderate negative association with better ear speech recognition in quiet scores (r=-0.438, 95% CI -0.701 to -0.069, P=.022).
At the end of the two hours of paired comparison listening that we conducted in the sound treated auditorium, we surveyed the participants (n=27) regarding their likelihood of purchasing hearing aids with telecoil functionality and using hearing loops on their own in the future. Results of the survey are shown in Figure 7. Notably, 92.9 percent of the participants in the BTE group indicated that they would be ‘Very likely’ to use hearing loops in the future, while 84.6 percent of the participants in the CIC group indicated that they were either ‘Somewhat likely’ or ‘Very likely’ to do so.
Based on our findings, we believe the candidacy for both telecoils and remote microphone accessories is greater than what many clinicians previously thought. Inevitably, some patients will find greater benefit from using HAT than others, but there does not appear to be a clear correlation with the standard audiometric test battery; therefore, we strongly encourage trial of HAT for patients with either a measured SNR loss or a perceived hearing handicap that would be great enough to warrant the use of hearing aids.
Discussion
In our studies, we found that use of remote microphones and hearing loops each significantly improved distant speech recognition in noise when compared to hearing aids alone. Our participants, who used either CIC or Power Plus BTE style hearing aids, strongly preferred the telecoil function in combination with a hearing loop over listening with the standard hearing aid microphone setting for various types of audio, even in an auditorium with professional sound design. These observations validate the recommendation of assistive listening systems for hearing aids, even for individuals with more mild degrees of hearing loss. We also found that even brief in-office demonstrations and counseling regarding use of HATs with hearing aids appeared to have improved participant awareness and information retention, but greater exposure to comparative listening experiences may be necessary to motivate routine use. These results underscore the importance of counseling and in-office demonstrations of how to utilize these systems with hearing aids. Encouraging patients to make their own paired-comparison evaluations, in realistic scenarios, may improve perceived benefit of using HATs and lead to lasting behavior changes. ■
References
- Ding, Y., Chourasia, A., Anson, D., Atkins, T., & Vanderheiden, G. (2015). Understanding Decision Requirements for Selection of Assistive Technology. Proceedings of the Human Factors and Ergonomics Society Annual Meeting, 59(1), 160–164. https://doi.org/10.1177/1541931215591033
- Kaufmann, T., Sterkens, J., & Woodgate, J. M. (2015). The Preferred Assistive Listening Technology.
J. Audio Eng. Soc.
, 63(4), 5. - Killion, M. C., Niquette, P. A., Gudmundsen, G. I., Revit, L. J., & Banerjee, S. (2004). Development of a quick speech-in-noise test for measuring signal-to-noise ratio loss in normal-hearing and hearing-impaired listeners. The Journal of the Acoustical Society of America, 116(4), 2395–2405. https://doi.org/10/c4txzj
- Lopez, S. M., & Caccavo, M. T. (2014). How to Win Patients and Influence Community Communication: A Step by Step Guide for Looping your Community. Audiology Practices. https://www.audiologypractices.org/how-to-win-patients-and-influence-community-communication-a-step-by-step-guide-for-looping-your-community
- Rodemerk, K. S., & Galster, J. A. (2015). The Benefit of Remote Microphones Using Four Wireless Protocols. Journal of the American Academy of Audiology, 26(8), 724–731. https://doi.org/10.3766/jaaa.15008
- Turton, L., Souza, P., Thibodeau, L., Hickson, L., Gifford, R., Bird, J., Stropahl, M., Gailey, L., Fulton, B., Scarinci, N., Ekberg, K., & Timmer, B. (2020). Guidelines for Best Practice in the Audiological Management of Adults with Severe and Profound Hearing Loss. Seminars in Hearing, 41(03), 141–246. https://doi.org/10.1055/s-0040-1714744
- Van Engen, K. J., & Peelle, J. E. (2014). Listening effort and accented speech. Frontiers in Human Neuroscience, 8. https://doi.org/10.3389/fnhum.2014.00577
Authors’ Note: A portion of these results was presented at the annual meeting of the American Academy of Audiology held from 30 March to 2 April 2022 in St. Louis, MO and the annual convention of the Hearing Loss Association of America held from 23 to 25 June 2022 in Tampa, FL. A portion of the results will also be presented at the 66th International Congress of Hearing Aid Acousticians held from 12 to 14 October 2022 in Hanover, Germany.
Justin R. Burwinkel, Au.D is a Senior Research Audiologist at Starkey. Dr. Burwinkel’s research has investigated the perceptual effects of increased audio processing delay in adverse listening conditions, which has helped to guide the development of emerging noise reduction and speech enhancement techniques, as well as the deployment of wireless assistive listening technology. In addition, he has filed numerous patents for inventions relating to hearing aid connectivity, artificial intelligence, and fall risk management.
Maddie Olson, Au.D joined Starkey Hearing Technologies as a Research Audiologist in 2021. She organizes product validation efforts to evaluate hearing technologies prior to market release, ensuring patients' needs are being met. Additionally, Dr. Olson evaluates device efficacy over the lifetime of hearing aids, allowing for longitudinal assessment of patient benefit, through post-market studies. She is particularly interested in areas of research that help to investigate long-term, positive patient outcomes for hearing aid users.
Lori Rakita joined Starkey Hearing Technologies in 2021 as the Director of Clinical Research and was responsible for the output of the Research Department and organizing efforts related to product and feature development, validation, and studies that answer key audiological questions. Prior to Starkey, Dr. Rakita led teams in industry and medical settings in research efforts related to hearing aid performance, the effectiveness of signal processing, and the needs of individuals with hearing loss.
